No Babies Were Harmed in The Making of This Blog
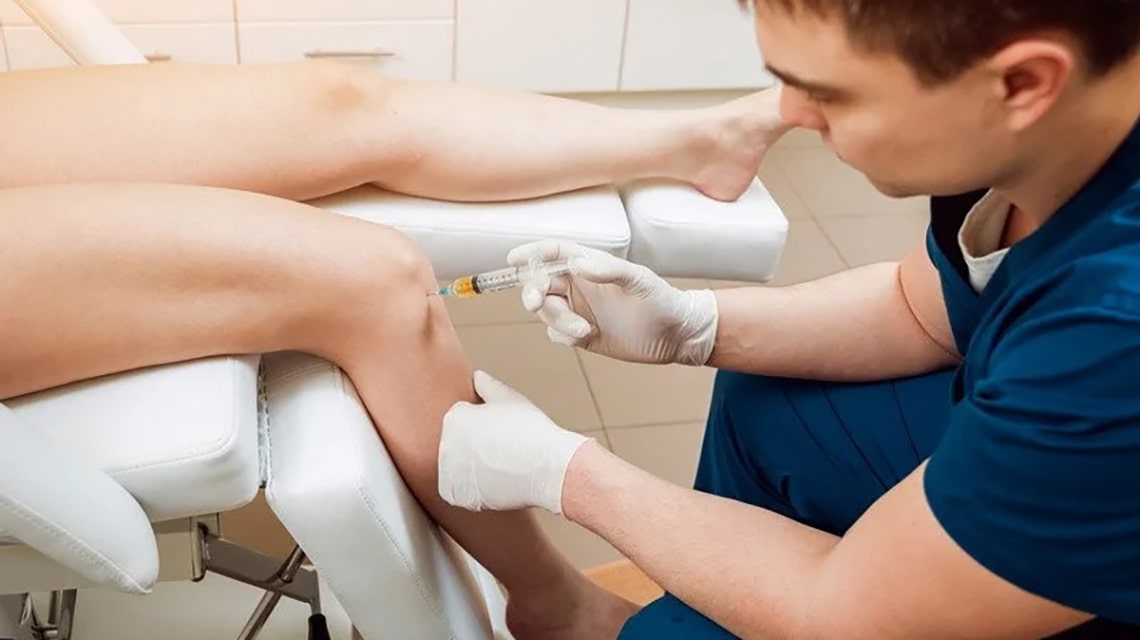
Placental tissues have been used as biologic dressings for over 100 years. Today, these total nucleated cells derived from the amniotic fluid

and membrane are being used in a broad range of clinical applications. These include the treatment of complex chronic pain, acute pain, and localized areas of injury or inflammation.
Placental tissues have been found to be a rich source of mesenchymal total nucleated cells, proteins, carbohydrates, hyaluronic acids and growth factors essential for fetal growth and development.
Amniotic tissue, the innermost layer of the placenta, is unique in that it is “immune-privileged” and, as such, rarely evokes an immune response in the human body. Research has shown that amniotic tissue does not express the Class II antigens that typically evoke an immune response. In addition, this tissue has been shown to have anti-inflammatory, anti-microbial and anti-adhesive properties. The collagens in the amniotic tissue provide a structural tissue matrix for cellular attachment. While providing structural support to cells, the extracellular matrix assists in the migration and proliferation of the patient’s own cells to the site of injury or defect.
The cells inherent in the placental tissues have been found to be broadly multipotent, capable of differentiating into adipogenic, osteogenic, myogenic, endothelial, neurogenic and hepatic cell lineages.
Placental tissue-derived allografts are a natural alternative to synthetic, cadaveric or animal derived regenerative products.
Amniotic total nucleated cells are derived from living, healthy donors who are pre-screened during pregnancy and selected based on stringent donor selection criteria. From aseptic recovery of the tissue at childbirth to timely processing and cryopreservation, our protocols and procedures have been developed to meet or exceed all applicable industry standards for the use of human cellular and tissue-based products.
#amnioticfluid #ApexBiologix #placentaltissue #alograftsamnioticstemcells #apex #amniotictissue
-3.jpg?width=693&height=225&name=Apex%20Logo%20(NEW%20-w-o%20gradient)-3.jpg)